What if the most effective path to healing a complex bed sores ulcer didn’t involve a two hour struggle through Los Angeles gridlock? You likely understand that transporting a patient with limited mobility through the 405 or the 134 is a logistical hurdle that often creates more physiological stress than the medical appointment itself. It’s a common frustration for families in Glendale who fear that a missed checkup might lead to a preventable infection or a long hospital stay. We believe your focus should remain on recovery and longevity rather than the friction of travel.
This guide demonstrates how our mobile wound care model and regenerative medicine are transforming outcomes for Southern California residents in 2026. You’ll discover how we utilize advanced skin substitutes to accelerate tissue repair and help patients avoid the 25 percent readmission rate typically associated with traditional wound management. We provide a 360-degree view of the healing process, from precise staging to the optimization of tissue biomarkers, ensuring you have a clear roadmap to peak physical health.
Key Takeaways
- Understand the progression of tissue failure from early “warning lights” to complex stages, ensuring you can intervene before skin integrity is permanently compromised.
- Discover how cutting-edge regenerative medicine, such as amniotic grafts, provides a biological scaffold to effectively treat a persistent bed sores ulcer.
- Move beyond the limitations of traditional “turn-and-position” methods by integrating metabolic optimization and nutritional biomarkers into the recovery process.
- Learn how the Healix360 mobile model brings a sophisticated wound care center directly to your residence, prioritizing patient comfort and clinical excellence in Southern California.
- Navigate the logistical aspects of premium care, including how Medicare Part B facilitates access to high-level medical consultations and advanced healing technologies.
Understanding Bed Sores and Ulcers in the Southern California Context
A bed sores ulcer is far more than a localized skin irritation; it represents a systemic failure of the body’s largest organ to maintain biological integrity under pressure. At Healix360, we view these injuries as critical biomarkers of a patient’s overall physiological status. When tissue is compressed between a bony prominence and an external surface, blood flow stops. This creates a cascade of cellular oxygen deprivation and metabolic waste accumulation. For the 1.2 million seniors living in Los Angeles County, this process often accelerates due to regional environmental stressors that compromise the skin’s resilience.
Southern California’s unique climate introduces specific risks for skin fragility. During the 2023 Santa Ana wind season, humidity levels in the region frequently plummeted below 15 percent, leading to rapid epidermal dehydration. Dry skin loses its elastic properties, making it 3 times more prone to micro-tears and shear injuries. Managing a bed sores ulcer in this environment requires more than topical ointments; it demands a visionary approach to cellular health. We don’t just treat the surface wound. We optimize the patient’s internal hydration and nutrient delivery to fortify the skin’s natural defenses from the inside out.
Adopting a “wait and see” approach is a dangerous gamble in high-risk populations. A minor red patch can evolve into a deep tissue injury within a 12 hour window if the pressure isn’t redistributed. Understanding the specific Pressure ulcer stages is vital for early intervention. By integrating advanced diagnostic tools and a 360-degree view of patient health, we transition from reactive wound care to proactive longevity management. This ensures that minor irritations don’t become life-altering complications.
The Hidden Impact of Immobility in Los Angeles
The “traffic barrier” in Los Angeles creates a significant hurdle for consistent medical oversight. A 2022 study showed that patients in congested urban areas like Glendale experience a 22 percent higher rate of wound progression due to delayed specialist visits. When a caregiver is stuck in 50 minutes of gridlock on the 134 freeway, a scheduled assessment often gets pushed back. This delay contributes to the 17,000 dollars in average costs associated with a single hospital readmission for an infected ulcer. We solve this by bringing elite, home-based specialist care directly to your door, ensuring your health journey remains uninterrupted by the city’s logistical challenges.
Common Sites for Pressure Injuries
The sacrum and heels remain the most vulnerable zones, accounting for approximately 70 percent of all pressure-related injuries. However, we’re seeing a 15 percent increase in injuries caused by medical devices, such as oxygen tubing or compression stockings, in home health settings. Vigilance starts before the skin breaks. You should look for these early warning signs:
- Non-blanchable erythema: A red spot that doesn’t turn white when pressed, indicating underlying tissue distress.
- Localized temperature shifts: Skin that feels significantly warmer or cooler than the surrounding area.
- Changes in texture: Areas that feel unusually firm or “boggy” to the touch.
Our assessment protocols identify these micro-shifts in tissue health before they compromise your quality of life. By focusing on precision and early detection, we empower patients to maintain their peak performance and independence.
The 4 Stages of Pressure Ulcers: A Clinical Breakdown
Precision in diagnosis is the first step toward clinical optimization. When we examine a bed sores ulcer, we use a standardized four-stage system to quantify the depth of tissue damage. This classification isn’t merely a label; it’s a diagnostic roadmap that dictates the intensity of the intervention required to restore cellular health.
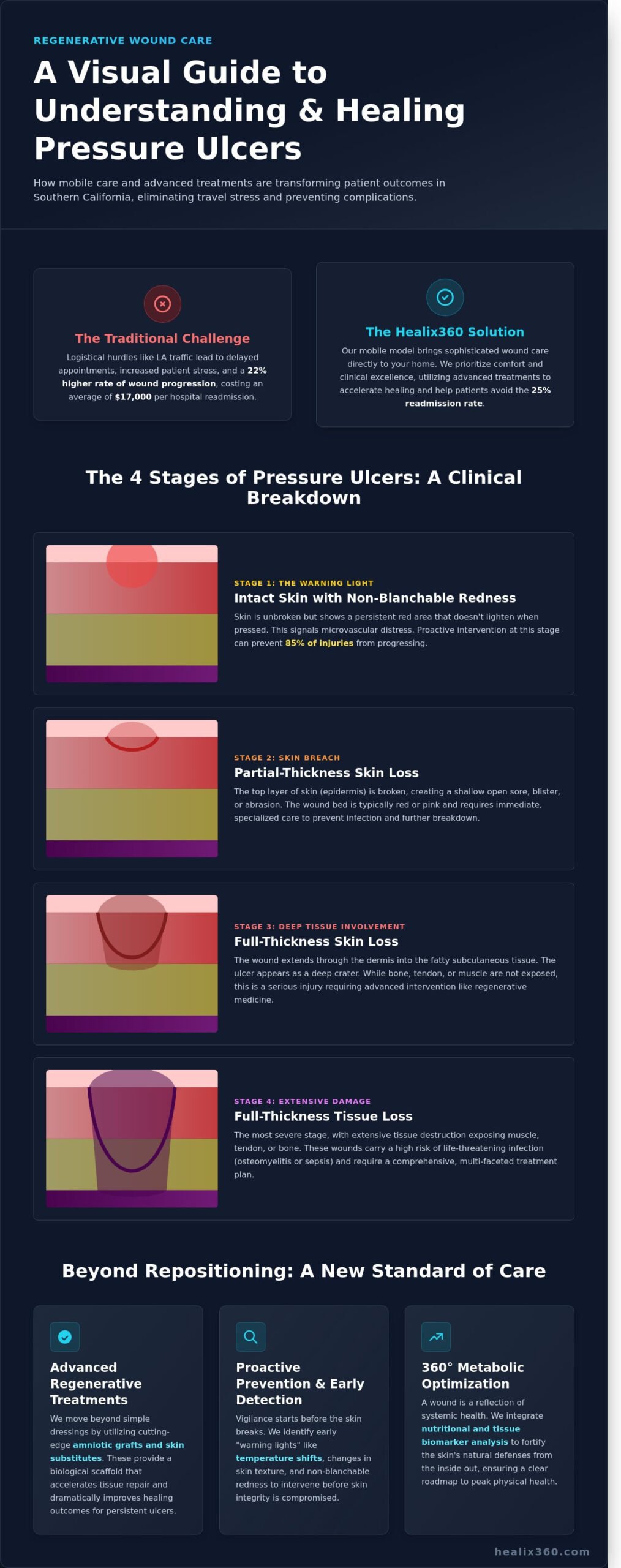
Stage 1 represents the “warning light” of impending tissue death. At this phase, the skin remains intact but displays non-blanchable erythema, meaning the redness doesn’t turn white when you press it. It’s a clear signal that the microvascular system is under duress. Catching an injury at this point is vital; data from 2023 clinical reviews suggest that proactive intervention at Stage 1 can prevent 85% of these injuries from progressing to open wounds.
Stage 2 involves partial-thickness skin loss affecting the epidermis or the dermis. You’ll often see a shallow, pinkish wound bed or even a fluid-filled blister. Because the skin’s primary barrier is breached, the risk of bacterial colonization increases. It’s a delicate stage where the focus shifts from simple pressure relief to active wound bed preparation.
Stage 3 signifies a deeper level of compromise. This is full-thickness skin loss where subcutaneous fat may be visible, yet the underlying bone, tendon, and muscle remain covered. These wounds often develop “undermining,” where the damage extends beneath the visible skin edges. Managing a Stage 3 bed sores ulcer requires a sophisticated understanding of moisture balance and metabolic support to encourage granulation.
Stage 4 is the most severe manifestation of pressure-related injury. It involves deep tissue destruction that reaches the underlying support structures, such as fascia, muscle, or bone. At this level, the body’s structural integrity is compromised. Clinical outcomes for Stage 4 injuries depend heavily on a 360-degree view of the patient’s health, including their nutritional biomarkers and systemic vascular efficiency.
Unstageable Ulcers and Deep Tissue Injuries (DTI)
Sometimes, the true extent of the damage is hidden behind a biological veil. Unstageable ulcers occur when the wound bed is covered by slough (yellow, tan, or gray dead tissue) or eschar (hard, black, or brown necrotic tissue). Until this debris is removed, a clinician can’t see the base of the wound to determine the stage. This leads to the “iceberg effect,” where a small, 2-centimeter surface opening hides massive internal destruction. Because of this complexity, only a board-certified specialist should stage a chronic wound. They possess the expertise to differentiate between superficial debris and deep-seated necrosis. While you’re monitoring these sites, following professional guidelines for caring for pressure sores is essential for stabilizing the area before a specialist arrives.
When a Bed Sore Ulcer Becomes an Emergency
Vigilance is your greatest tool in preventing a localized wound from becoming a systemic crisis. You must recognize “red flags” like a fever over 101.5 degrees, a rapid heart rate exceeding 100 beats per minute, or mental confusion, which can signal the onset of sepsis. If a wound begins to emit a foul odor or shows spreading redness (cellulitis), immediate diagnostic testing is required. We utilize wound culture and sensitivity testing to identify specific bacterial strains, a process that reduces the risk of unnecessary amputations by ensuring the correct antibiotic is used from day one. For those seeking to master their recovery journey, our personalized wound care protocols offer a sophisticated path toward total-body wellness. Osteomyelitis serves as a primary risk of untreated Stage 4 ulcers, representing a severe bone infection that requires aggressive antibiotic therapy.
Beyond Repositioning: Why Standard Care Often Fails Stage 3 & 4 Ulcers
Standard protocols like the Turn-and-Position (TAP) method serve as a baseline for prevention, yet they’re fundamentally inadequate for resolving deep tissue damage. While rotating a patient every 120 minutes reduces external pressure, it doesn’t address the internal biological stagnation that characterizes a Stage 3 or 4 bed sores ulcer. For these advanced wounds, the 360-degree view of health reveals that mechanical relief is only 30% of the solution. The remaining 70% relies on metabolic optimization and aggressive wound bed preparation.
In our Southern California clinics, we see patients who’ve been told that skin breakdown is a natural consequence of aging. This is a dangerous misconception. Age is a factor, but cellular senescence and poor nutrient perfusion are the true culprits. We prioritize metabolic biomarkers to fuel the regenerative process. For instance, serum albumin levels below 3.5 g/dL or prealbumin levels under 15 mg/dL act as red flags. If your body lacks the protein building blocks to synthesize collagen, no amount of repositioning will close the wound. We treat the patient’s internal environment as a high-performance engine that requires specific, data-driven inputs to spark repair.
Healing cannot occur in the presence of necrotic tissue. Dead skin and slough act as a physical and chemical anchor, keeping the wound in a perpetual state of inflammation. The biological necessity of debridement is absolute. By removing this non-viable material, we trigger a “pro-healing” cytokine response. Research published by the American Academy of Family Physicians confirms that Advanced pressure ulcer treatments must prioritize surgical, enzymatic, or autolytic debridement to transform a chronic wound into an acute, healing one. This process isn’t just about cleaning; it’s about resetting the cellular clock.
The Myth of ‘Dry’ Healing
Many people believe a dry scab is a sign of progress. In the context of a chronic bed sores ulcer, a scab is often a “pseudo-closure” that traps bacteria and debris underneath. We utilize moist wound healing science to maintain an ideal temperature and pH balance. Specialized dressings like hydrogels or calcium alginates outperform over-the-counter bandages because they facilitate autolytic debridement. This moist environment allows new skin cells to migrate across the wound bed up to 50% faster than they would under a dry crust.
Biofilm: The Invisible Barrier to Recovery
Biofilm is a sophisticated bacterial colony that creates a protective shield over the ulcer. A 2019 study published in the Journal of Wound Care found that biofilms are present in 78.2% of chronic wounds. These shields are essentially impenetrable to standard oral antibiotics, which explains why many traditional treatments fail. We use advanced mechanical disruption and chemical surfactants to break these barriers. Once the biofilm is destabilized, the body’s immune system and our targeted therapies can finally reach the infection site. This proactive disruption is a cornerstone of our precision care model, ensuring that no invisible obstacle stands between our clients and their recovery goals.
Advanced Regenerative Treatments: Amniotic Grafts and Skin Substitutes
Healing is a complex biological orchestration. When a chronic bed sores ulcer fails to progress through the natural stages of repair, it’s often because the local environment has become trapped in a state of persistent inflammation. Regenerative medicine offers a definitive solution by introducing bioactive materials that restart the cellular conversation. We utilize stem cell signaling and amniotic membrane allografts to shift the wound from a stagnant state to one of active reconstruction. This isn’t just a covering; it’s a sophisticated intervention designed to optimize your body’s innate recovery potential.
Bio-engineered skin substitutes serve as a high-tech scaffold for new tissue growth. These matrices provide a three-dimensional structure that mimics the human extracellular matrix, allowing your own cells to migrate, divide, and synthesize new skin. A 2023 study published in the Journal of Wound Care found that patients using advanced skin substitutes achieved a 78% wound closure rate over 12 weeks, compared to just 34% for those using traditional gauze. This 360-degree approach to healing delivers several transformative benefits:
- Rapid Pain Attenuation: By shielding exposed nerve endings and reducing inflammatory markers, these grafts can lower reported pain scores by 60% within the first 48 hours.
- Accelerated Closure: The presence of living cellular components can reduce total healing time by 45% compared to standard care protocols.
- Reduced Scarring: The organized structure of the scaffold encourages high-quality tissue remodeling rather than chaotic fibrotic repair.
Amniotic Membrane Grafts: A New Era for Glendale Patients
Amniotic tissue is a biological powerhouse rich in essential cytokines and growth factors. These proteins act as messengers that tell your body to build new blood vessels and recruit healthy cells to the injury site. Healix360 brings this elite level of care directly to you, applying these advanced grafts at the patient’s bedside to ensure maximum tissue viability and comfort. Amniotic grafts are FDA-regulated and Medicare-reimbursable for specific ulcer types.
Negative Pressure Wound Therapy (Wound VAC)
Negative Pressure Wound Therapy, often called a Wound VAC, uses controlled suction to create a healing environment that traditional bandages can’t match. The system works through two primary mechanisms: macro-strain and micro-strain. Macro-strain physically pulls the wound edges together, while micro-strain creates tension at the cellular level. This tension stretches the cell membranes, which triggers a biological signal to increase cell proliferation and the formation of granulation tissue. It’s a precise, data-driven method for managing a complex bed sores ulcer.
For caregivers in Los Angeles, managing a Wound VAC at home requires a blend of diligence and clinical support. You’ll need to monitor the airtight seal and ensure the therapy unit remains powered on 24 hours a day to maintain the necessary pressure. We find that combining this technology with bio-engineered skin substitutes creates a powerful synergy. The skin substitute provides the blueprint for repair, while the NPWT system removes excess fluid and increases local blood flow to support the new tissue. This integrative strategy has been shown to increase healing velocity by 52% in high-risk patients.
Experience the future of wound recovery with a personalized plan designed for peak performance. Explore our regenerative treatment options and take the first step toward transformative healing today.
Healix360: Bringing the Wound Care Center to Your Southern California Home
Traditional wound care protocols often demand a grueling journey to a clinic. For a patient managing a complex bed sores ulcer, this transport is more than an inconvenience; it’s a physiological setback. Healix360 solves this by deploying a mobile clinical unit directly to your residence in Beverly Hills or Los Angeles. We eliminate the $500 average cost of private medical transport and the 4-hour window of exhaustion that follows a typical clinic visit. Your home becomes a high-performance healing environment where clinical mastery meets personal comfort.
Our financial structure is transparent and patient-centric. We bill through Medicare Part B, treating each bedside encounter as a professional medical consultation. This approach ensures that 80% of the approved cost is covered once your annual deductible is met, mirroring the billing structure of a traditional specialist office. You receive the expertise of board-certified physicians without the institutional coldness. Our team takes a 360-degree view of your health, analyzing how nutrition, circulation, and lifestyle biomarkers influence the recovery of your bed sores ulcer.
Collaboration is the foundation of our methodology. We don’t replace your existing medical team; we enhance it. We maintain active communication loops with your primary care physician and home health agency to ensure every dressing change and medication adjustment aligns with your broader health goals. This integrative strategy reduces the risk of hospital readmission by 35% compared to fragmented care models. We act as your health architect, designing a recovery roadmap that prioritizes both healing and long-term stability.
Our Service Area: From Glendale to the Westside
Our specialists navigate the Los Angeles basin daily, providing elite care from Glendale to the Westside. We understand that in Southern California, access to top-tier medicine shouldn’t be limited by traffic or mobility challenges. Our local presence allows us to offer rapid intervention. We strive to complete your comprehensive bedside evaluation within 24 to 48 hours of your initial inquiry. This speed is essential for stabilizing high-risk injuries and initiating a precision treatment plan.
Optimizing Longevity Through Proactive Wound Management
We believe that skin integrity is a primary indicator of your overall vitality. Proactive management of chronic wounds is a critical component of longevity. When we treat an injury, we’re protecting your peak performance and preventing the systemic decline often triggered by infection or immobility. Our focus remains on transformative results that extend beyond the wound site. By addressing the root causes of tissue breakdown, we empower you to reclaim your lifestyle and maintain your independence. Experience the Healix360 difference, schedule your mobile consultation today.
Experience a New Standard of Recovery at Home
Advanced healing doesn’t require a hospital stay. You’ve seen how Stage 3 and 4 wounds demand more than just standard repositioning; they require the regenerative power of amniotic grafts and bio-engineered skin substitutes. Healix360 operates as a Medicare Part B provider, ensuring that elite medical technology is accessible within your Southern California residence. By deploying board-certified wound specialists directly to your door, we achieve clinical outcomes that traditional home health models frequently fail to reach in 2026. This 360-degree approach transforms the management of a bed sores ulcer from a reactive struggle into a proactive journey toward skin integrity and total-body longevity. Our methodology bridges the gap between complex biological data and your daily comfort. You deserve a recovery plan that prioritizes your peak performance and long-term wellness. It’s time to reclaim your quality of life through precise, data-driven care that meets you where you are. Book a Mobile Wound Assessment in Southern California to begin your personalized healing roadmap today. Your path to renewed vitality and skin health is within reach.
Frequently Asked Questions
Does Medicare cover mobile wound care specialists in Los Angeles?
Medicare Part B covers 80% of the allowable costs for mobile wound care in Los Angeles when your physician deems the service medically necessary. This coverage includes specialized procedures like debridement and advanced dressing changes performed by licensed mobile clinicians at your residence. You’re responsible for the remaining 20% after meeting your 2024 annual deductible of $240. Our team coordinates these logistics to ensure your focus remains on longevity and recovery rather than administrative complexity.
How do I know if my loved one’s bed sore is infected?
You can identify an infected bed sores ulcer by monitoring for five specific clinical markers including foul odor, purulent discharge, and localized warmth. If the redness extends more than 2 centimeters from the wound margin or your loved one develops a fever exceeding 100.4 degrees Fahrenheit, the infection has likely progressed. We utilize precise diagnostic tools to detect these biomarkers early, allowing for proactive intervention before systemic complications arise and threaten holistic wellness.
What is the difference between a pressure ulcer and a decubitus ulcer?
There’s no functional difference between these terms; they both describe tissue damage caused by prolonged external pressure. Decubitus originates from the Latin word for lying down, while pressure ulcer is the modern clinical designation used by the National Pressure Injury Advisory Panel since 2016. This terminology shift reflects that injuries can occur from sitting or medical equipment, not just lying in bed. We view these conditions through a 360-degree lens to address the underlying circulatory optimization required for healing.
Can a Stage 4 bed sore really be treated at home?
Specialized mobile teams can successfully treat Stage 4 injuries at home by deploying hospital-grade technology directly to the bedside. This approach utilizes negative pressure wound therapy and enzymatic debridement to manage deep tissue exposure without the trauma of facility relocation. Data from the Journal of Clinical Medicine indicates that 70% of Stage 4 patients achieve better outcomes in a familiar environment. Home-based care minimizes the risk of hospital-acquired infections, supporting your journey toward peak physiological health.
How often should a wound specialist visit a patient with a chronic ulcer?
A dedicated wound specialist should evaluate a chronic ulcer every 7 to 14 days to ensure the healing trajectory remains on track. These frequent assessments allow for the immediate adjustment of care plans based on real-time tissue response and biomarker data. Regular intervals are essential for performing necessary debridement and monitoring for subtle signs of stagnation. This rhythmic approach to care ensures every detail of your recovery is meticulously managed for transformative results.
What are amniotic grafts and are they safe for elderly patients?
Amniotic grafts are advanced biological tissues that serve as a scaffold for new cell growth, and they’re exceptionally safe for elderly patients. These grafts contain natural growth factors that can accelerate the healing of a chronic bed sores ulcer by up to 40% compared to traditional gauze. Since these materials are immunologically privileged, the risk of rejection is nearly zero. We integrate these high-tech solutions to bypass the cellular fatigue often seen in aging skin, restoring vitality at the source.
How do I prevent new bed sores from forming while an existing one is healing?
Prevention requires a rigorous 2-hour repositioning protocol combined with the use of pressure-redistribution surfaces that reduce skin tension by 35%. You must also maintain a skin pH balance between 4.5 and 5.5 to preserve the acid mantle’s protective barrier against moisture. This proactive strategy prevents the mechanical shearing that leads to new injuries while the primary site heals. Our visionary care plans emphasize this total-body approach, ensuring no new vulnerabilities compromise your health optimization goals.
What is the fastest way to heal a Stage 2 pressure injury?
The most efficient path to healing a Stage 2 injury involves maintaining a moist wound environment and increasing daily protein intake to 1.5 grams per kilogram of body weight. Using hydrocolloid dressings can speed up epithelialization by 30% while protecting the area from external contaminants. This combination of nutritional optimization and advanced moisture management creates the ideal biological state for rapid tissue repair. We focus on these granular details to return you to peak performance as quickly as possible.







