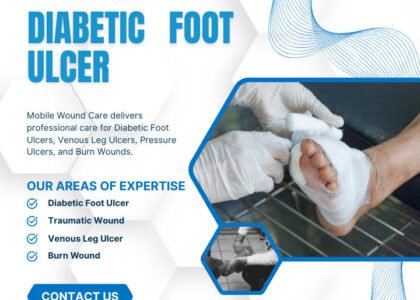
Moisture Balance in Wound Healing: Optimizing the Wound Environment for Effective Treatment
Moisture balance is a critical factor in wound healing, influencing the rate and quality of recovery. An optimal moisture environment promotes cellular activities essential for healing, such as granulation tissue formation and epithelialization. This article delves into the key factors that affect moisture levels in wounds, techniques for managing moisture, and the impact of moisture balance on healing outcomes. Additionally, we will explore the stages of wound healing and their specific moisture requirements, as well as best practices for managing chronic wounds. Understanding these elements is vital for healthcare providers and patients alike, as effective moisture management can significantly enhance healing processes.
Key Factors Influencing Moisture Levels:
Moisture levels in wounds are influenced by several key factors, including the type of wound, the selection of dressings, and the patient’s hydration status. Each of these elements plays a crucial role in determining the moisture balance necessary for optimal healing.
Wound Type and Exudate
Different types of wounds produce varying amounts of exudate, which directly affects moisture levels. For instance, heavily exuding wounds, such as those from burns or surgical sites, require specific dressings that can absorb excess fluid while maintaining a moist environment. Understanding the characteristics of wound exudate is essential for selecting appropriate dressings that support healing.
Dressing Selection
Choosing the right dressing is vital for effective moisture management. Various dressing types, such as hydrocolloid and alginate dressings, are designed to retain moisture while allowing for gas exchange. Hydrocolloid dressings, for example, are particularly effective in maintaining a moist wound environment, which is crucial for promoting healing and preventing infection.
Hydration Status
The systemic hydration status of a patient significantly impacts wound healing. Adequate hydration supports cellular functions and skin integrity, while dehydration can hinder recovery and lead to complications. Ensuring that patients maintain proper hydration levels is essential for optimizing the healing process.
Techniques for Managing Moisture:
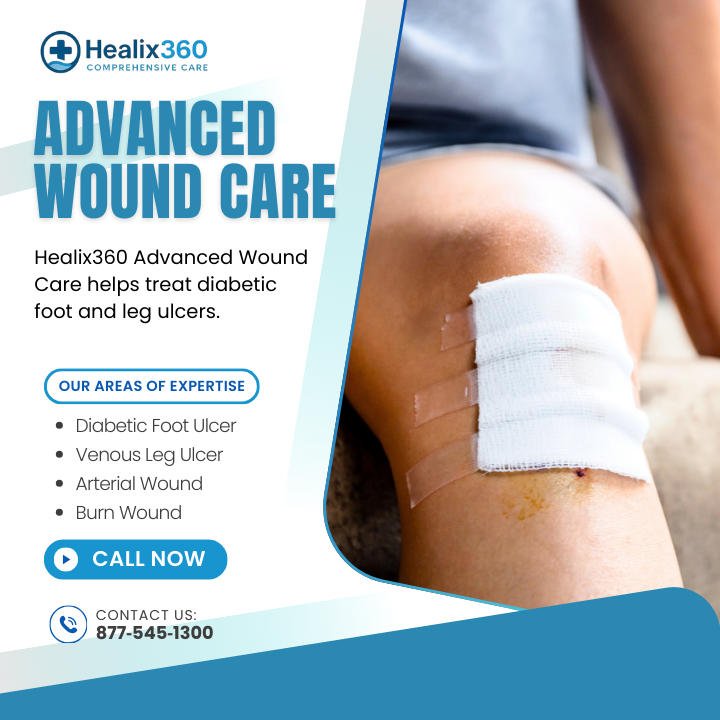
Effective moisture management involves several techniques that healthcare providers can implement to maintain optimal moisture levels in wounds. These techniques include regular dressing changes, the use of moisture-retentive dressings, and ongoing monitoring and assessment of the wound.
Regular Dressing Changes
Regular dressing changes are essential to prevent saturation and maintain moisture balance. The frequency of dressing changes should be based on the level of wound drainage and clinical guidelines. By adhering to these guidelines, healthcare providers can ensure that the wound remains in an optimal state for healing.
Moisture-Retentive Dressings
Moisture-retentive dressings are specifically designed to maintain a moist environment while managing exudate. These dressings, such as hydrocolloids and foams, provide a barrier against external contaminants while allowing for the absorption of excess fluid. Their use is critical in promoting healing and reducing the risk of infection.
Monitoring and Assessment
Regular monitoring and assessment of the wound are crucial for effective moisture management. Healthcare providers should assess for signs of infection and moisture imbalance, documenting any changes to track healing progress. This proactive approach allows for timely interventions and adjustments to the treatment plan as needed.
Impact on Healing Outcomes:
The balance of moisture in a wound significantly affects healing outcomes. A moist environment promotes faster healing, reduces the risk of infection, and enhances patient comfort. Understanding the relationship between moisture levels and healing outcomes is essential for optimizing treatment strategies.
For instance, studies have shown that wounds maintained in a moist environment heal more quickly than those that are allowed to dry out. This is due to the fact that moisture facilitates cellular migration and proliferation, which are critical processes in wound healing. Additionally, balanced moisture levels can help prevent complications such as maceration and infection, further supporting the healing process.
What Are the Key Stages of Wound Healing and Their Moisture Requirements?
Wound healing occurs in several distinct stages, each with specific moisture requirements. Understanding these stages is crucial for effective wound management.
How Does Moisture Influence Each Phase of Wound Healing?
Moisture plays a vital role in each phase of wound healing, including hemostasis, inflammation, proliferation, and maturation. During the inflammatory phase, moisture is critical for cellular migration and the formation of new tissue. In the proliferation phase, a moist environment supports the growth of granulation tissue and epithelial cells, while in the maturation phase, moisture levels must be carefully managed to ensure proper remodeling of the wound.
What Are the Clinical Indicators of Optimal Moisture Levels During Healing?
Clinical indicators of optimal moisture levels include the appearance of the wound, the amount of drainage, and the presence of granulation tissue. Healthcare providers should monitor these indicators closely to ensure that moisture levels are maintained within the ideal range for healing.
Which Moist Wound Dressings Best Maintain Optimal Moisture Balance?
Selecting the appropriate dressing is essential for maintaining moisture balance in wounds. Various types of dressings are available, each with unique properties that cater to different moisture management needs.
What Types of Moisture-Retentive Dressings Are Available?
Moisture-retentive dressings include hydrocolloid, alginate, and foam dressings. Each type serves specific purposes based on the wound’s characteristics:
These dressings are designed to create a moist environment that promotes healing while managing exudate effectively.
How Do Dressing Properties Affect Wound Exudate Management?
The properties of dressings significantly influence how they manage wound exudate. For example, dressings with high absorbency can effectively handle excess fluid, preventing maceration and maintaining a moist environment. Conversely, dressings that do not absorb adequately may lead to moisture imbalance, hindering the healing process.
How Can Infection Prevention Be Integrated into Moisture Management Protocols?
Infection prevention is a critical component of moisture management protocols. Maintaining an optimal moisture balance can help reduce the risk of infection, as excessively dry or overly moist environments can both contribute to complications. Patient education on proper wound care and hygiene practices is essential for effective infection prevention.
What Is the Relationship Between Moisture Levels and Infection Risk?
There is a direct relationship between moisture levels and infection risk in wound care. Balanced moisture levels can reduce the likelihood of infection, while excessive moisture can lead to maceration and create an environment conducive to bacterial growth. Therefore, careful monitoring and management of moisture levels are crucial for preventing infections.
Which Evidence-Based Practices Reduce Infection in Moist Wound Care?
Evidence-based practices for reducing infection in moist wound care include:
- Regular Wound Cleaning: Keeping the wound clean helps prevent infection.
- Timely Dressing Changes: Changing dressings as needed prevents saturation and maintains moisture balance.
- Patient Education: Educating patients on proper wound care techniques empowers them to manage their wounds effectively.
Implementing these practices can significantly enhance wound healing outcomes and reduce the risk of complications.
What Are Best Practices for Managing Chronic Wounds with Moisture Balance?
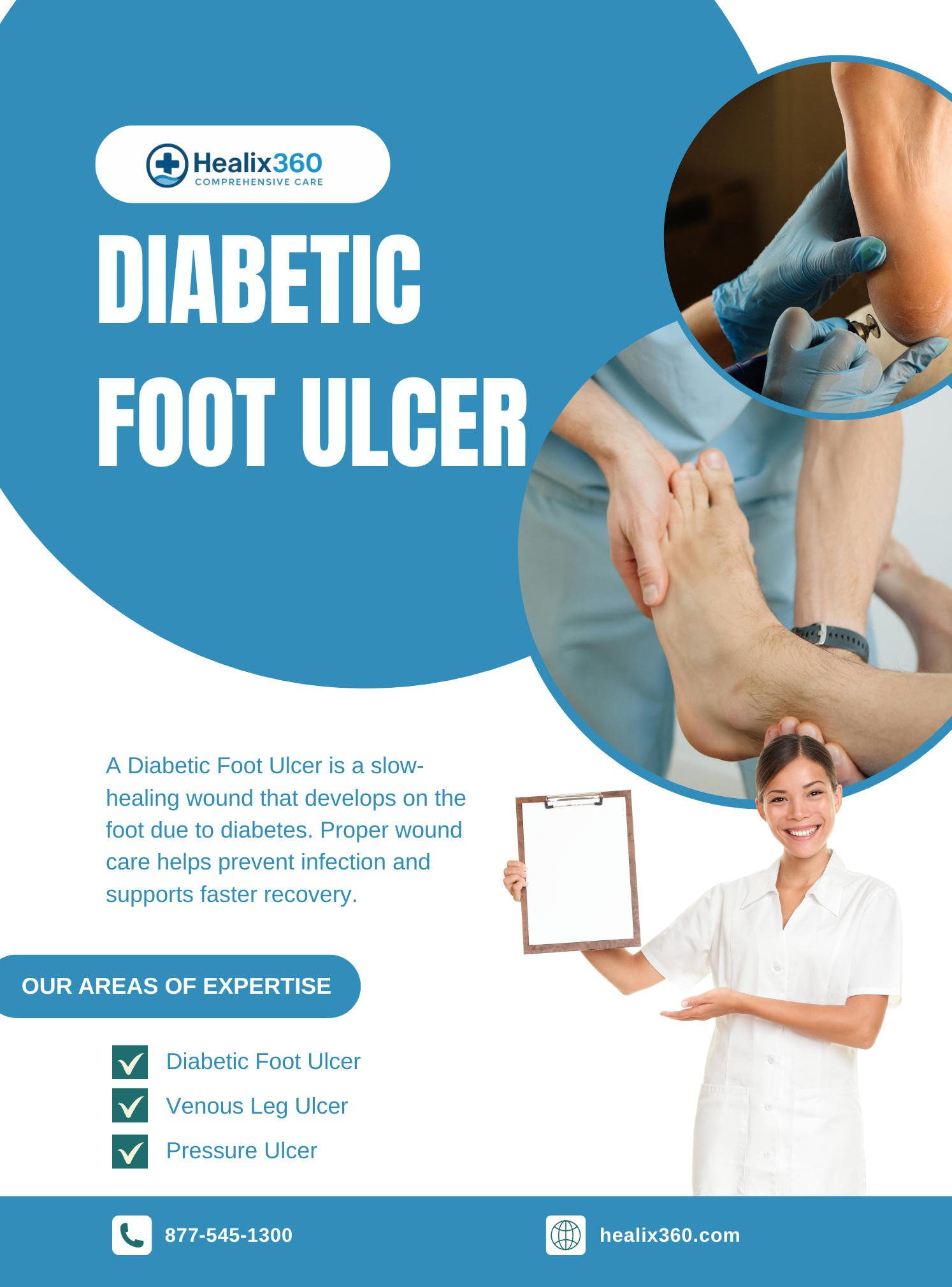
Managing chronic wounds requires a tailored approach that emphasizes moisture balance. Best practices include:
- Regular Assessments: Frequent evaluations of the wound’s condition help inform treatment decisions.
- Appropriate Dressing Selection: Choosing the right dressing based on the wound’s characteristics is essential for effective moisture management.
- Patient-Centered Care Plans: Developing personalized care plans that consider the patient’s unique needs and circumstances can improve healing outcomes.
How Does Moisture Management Differ in Chronic Versus Acute Wounds?
Moisture management strategies differ significantly between chronic and acute wounds. Chronic wounds often require long-term management and may necessitate more frequent assessments and adjustments to the treatment plan. In contrast, acute wounds typically heal more quickly and may require less intensive moisture management.
What Role Do Personalized Care Plans Play in Chronic Wound Healing?
Personalized care plans are crucial for chronic wound healing, as they allow healthcare providers to tailor treatment strategies to the individual patient’s needs. These plans should consider factors such as the patient’s overall health, the characteristics of the wound, and the patient’s preferences. Regular follow-ups are essential to ensure that the care plan remains effective and relevant.
How Can Home-Based Wound Care Support Optimal Moisture Balance?
Home-based wound care can significantly support optimal moisture balance by allowing for personalized treatment in a familiar environment. Patients can be educated on proper wound care techniques, enabling them to manage their wounds effectively at home. This approach can lead to improved healing outcomes and greater patient satisfaction.
What Are the Advantages of Moisture Management in Private Residences?
Moisture management in private residences offers several advantages, including:
- Personalized Care: Patients receive care tailored to their specific needs and preferences.
- Reduced Stress: Familiar environments can reduce anxiety and promote healing.
- Empowerment: Educating patients and caregivers on moisture management empowers them to take an active role in the healing process.
How Are Patient Referrals and Provider Partnerships Facilitated for Home Care?
Facilitating patient referrals and provider partnerships for home care is essential for ensuring comprehensive wound management. Strong partnerships between healthcare providers and home care agencies enhance care delivery and support optimal moisture management. Education and support for caregivers are key components of this collaborative approach, ensuring that patients receive the best possible care in their homes.
For more information on how “private residences” can improve wound care, contact us.