Wound Dressing Selection Guide: Choosing the Right Products for Optimal Healing Outcomes
Selecting the appropriate wound dressing is crucial for effective healing and recovery. With a variety of options available, understanding the different types of wound dressings and their specific applications can significantly impact patient outcomes. This guide aims to provide a comprehensive overview of wound dressing selection, focusing on the mechanisms, benefits, and clinical applications of various products. Many patients and healthcare providers face challenges in choosing the right dressings for chronic wounds, diabetic ulcers, and pressure injuries. By exploring the criteria for selection and the role of infection risk, this article will equip readers with the knowledge needed to make informed decisions. Key sections will cover the types of dressings, selection criteria, and best practices for application and maintenance.
Indeed, successful wound dressing selection requires a dynamic approach, adapting to the wound’s changing healing environment and specific characteristics.
Wound Dressing Selection: Types, Properties & Healing
Appropriate wound dressing selection is guided by an understanding of wound dressing properties and an ability to match the level of drainage and depth of a wound. Wounds should be assessed for necrosis and infection, which need to be addressed prior to selecting an ideal dressing. Moisture-retentive dressings include films, hydrogels, hydrocolloids, foams, alginates, and hydrofibers and are useful in a variety of clinical settings. Antimicrobial-impregnated dressings can be useful in wounds that are superficially infected or are at higher risk for infection. For refractory wounds that need more growth stimulation, tissue-engineered dressings have become a viable option in the past few decades, especially those that have been approved for burns, venous ulcers, and diabetic ulcers. As wounds heal, the ideal dressing type may change, depending on the amount of exudate and depth of the wound; thus success in wound dressing selection hinges on recognition of the changing healing environment.
Wound dressings: selecting the most appropriate type, 2013
What Are the Different Types of Wound Dressings and Their Clinical Applications?
Wound dressings are essential tools in managing various types of wounds, each designed to address specific healing needs. The primary types of dressings include hydrocolloid, foam, alginate, and antimicrobial dressings, each offering unique benefits based on the wound’s characteristics and healing stage.
Understanding these types allows healthcare providers to tailor their approach to individual patient needs, ensuring optimal healing outcomes.
How Do Hydrocolloid Dressings Support Moderate Exudate Wound Healing?
Hydrocolloid dressings are designed to maintain a moist environment, which is critical for the healing of moderate exudate wounds. They work by forming a gel-like substance when in contact with wound exudate, which helps to retain moisture and promote autolytic debridement. This moisture retention not only aids in healing but also reduces pain during dressing changes, making them a patient-friendly option. Additionally, hydrocolloid dressings can be left in place for extended periods, minimizing the frequency of changes and enhancing patient comfort.
What Are the Benefits of Foam and Alginate Dressings in Chronic Wound Management?
Foam and alginate dressings play a vital role in managing chronic wounds due to their unique properties. Foam dressings are highly absorbent, making them suitable for wounds with significant exudate. They provide cushioning and protection, which is essential for preventing further injury. Alginate dressings, on the other hand, are derived from seaweed and are particularly effective for highly exudative wounds. They form a gel upon contact with exudate, which not only absorbs moisture but also promotes hemostasis. Both dressing types are crucial in ensuring a conducive healing environment for chronic wounds.
Among the diverse options, foam dressings stand out for their adaptability and wide range of applications in managing persistent wounds.
Foam Dressings in Chronic Wound Management
They are some of the most variable and versatile dressings for chronic wound care and include thin and thick foams, adhesive and nonadhesive foams, foams used to pack wounds, and foams combined with other dressing types.
Dressing selection in chronic wound management, 2002
Given the dynamic nature of chronic wounds, selecting the most appropriate dressing is a critical decision that significantly impacts patient recovery and resource utilization.
Choosing Wound Dressings for Optimal Healing
Chronic wounds are frequently dynamic in presentation, and the numerous wound dressings available make dressing selection challenging for the practitioner. Choosing the correct dressing for a particular wound type is critical for optimal healing outcomes and can significantly reduce treatment costs and patient discomfort.
Choosing a wound dressing based on common wound characteristics, 2016
Which Criteria Should Guide the Selection of Appropriate Wound Dressings?
Selecting the right wound dressing involves considering several critical factors. These include the type of wound, the level of exudate, the healing stage, and the risk of infection. Each of these criteria plays a significant role in determining the most effective dressing for a given situation.
- Wound Type: Different wounds, such as surgical, traumatic, or chronic, require specific dressing types to promote healing.
- Exudate Level: The amount of fluid produced by the wound influences dressing choice; high-exudate wounds need more absorbent dressings.
- Healing Stage: The phase of healing (inflammatory, proliferative, or maturation) dictates the dressing’s properties needed for optimal recovery.
By evaluating these criteria, healthcare providers can make informed decisions that enhance healing and reduce complications.
How Does Wound Type and Exudate Level Influence Dressing Choice?
The characteristics of the wound, including its type and the level of exudate, are paramount in guiding dressing selection. Acute wounds, such as surgical incisions, may require different management compared to chronic wounds like diabetic ulcers. For instance, a surgical wound with minimal exudate may benefit from a simple adhesive dressing, while a chronic wound with high exudate may necessitate a more absorbent foam or alginate dressing. Understanding these dynamics ensures that the chosen dressing aligns with the wound’s needs, promoting effective healing.
What Role Does Infection Risk Play in Dressing Selection?
Infection risk is a critical consideration in wound dressing selection. Wounds that are at a higher risk of infection, such as those with necrotic tissue or significant exudate, may require antimicrobial dressings. These dressings contain agents that help prevent bacterial growth and reduce the likelihood of infection. Regular assessment of the wound for signs of infection, such as increased redness, swelling, or discharge, is essential in determining the need for antimicrobial intervention. By prioritizing infection control, healthcare providers can enhance patient outcomes and facilitate faster healing.
How Should Wound Dressings Be Applied and Maintained for Effective Healing?
Proper application and maintenance of wound dressings are vital for ensuring effective healing. Following best practices can significantly reduce the risk of complications and promote optimal recovery.
- Preparation: Clean the wound area thoroughly before applying the dressing to prevent contamination.
- Application Techniques: Use sterile techniques to apply the dressing, ensuring it adheres well without causing trauma to the wound.
- Monitoring: Regularly check the dressing for signs of leakage or infection, and change it as needed to maintain a clean and moist environment.
What Are the Best Practices for Dressing Application Techniques?

Effective dressing application techniques are crucial for wound healing. Start by washing hands thoroughly and using sterile gloves. Clean the wound with saline or an appropriate antiseptic solution, ensuring that all debris is removed. Apply the dressing gently, avoiding tension that could disrupt the healing tissue. Secure the dressing adequately to prevent movement, which can lead to irritation or injury. Following these steps helps create an optimal healing environment.
How Often Should Dressings Be Changed to Prevent Infection?
The frequency of dressing changes depends on several factors, including the type of dressing used, the level of exudate, and the wound’s condition. Generally, dressings should be changed when they become saturated or if there are signs of infection. For hydrocolloid dressings, changes may be less frequent, while foam and alginate dressings may require more regular changes due to higher absorbency needs. Monitoring the wound closely is essential to determine the appropriate change schedule.
What Are the Advantages of Advanced and Antimicrobial Wound Dressings?

Advanced and antimicrobial wound dressings offer several advantages over traditional options. These dressings are designed to provide enhanced protection and promote faster healing through their specialized properties.
- Infection Prevention: Antimicrobial dressings contain agents that actively combat bacterial growth, reducing the risk of infection.
- Enhanced Healing: Many advanced dressings are engineered to maintain optimal moisture levels, which is crucial for effective healing.
- Cost-Effectiveness: While they may have a higher upfront cost, the potential for reduced complications and faster healing can lead to overall cost savings.
How Do Antimicrobial Dressings Prevent Wound Infection?
Antimicrobial dressings work by releasing active agents that inhibit bacterial growth. These agents can include silver, iodine, or honey, each with unique mechanisms of action. By creating an environment that is hostile to bacteria, these dressings help prevent infection and promote healing. Clinical studies have shown that the use of antimicrobial dressings can significantly reduce infection rates in high-risk wounds, making them a valuable tool in wound management.
What Clinical Evidence Supports the Use of Bioactive Dressings?
Recent clinical trials have demonstrated the effectiveness of bioactive dressings in promoting wound healing. These dressings often contain growth factors or other bioactive substances that stimulate cellular activity and tissue regeneration. Evidence suggests that patients using bioactive dressings experience faster healing times and improved outcomes compared to those using standard dressings. This emerging research supports the integration of bioactive options into wound care protocols.
How Do Cost and Insurance Considerations Affect Wound Dressing Selection?
Cost and insurance coverage are significant factors influencing wound dressing selection. Advanced dressings may come with higher price tags, which can be a barrier for some patients. Understanding insurance policies and potential out-of-pocket costs is essential for both patients and providers. Many insurance plans cover specific types of dressings, but coverage can vary widely. Providers should be prepared to discuss these aspects with patients to ensure they receive the most appropriate care within their financial means.
Where Can Patients and Providers Access Resources and Support for Wound Dressing Selection?
Access to resources and support is vital for effective wound care management. Patients and healthcare providers can benefit from educational materials, professional organizations, and online communities that focus on wound care. These resources can provide valuable information on the latest advancements in wound dressing technologies and best practices for application and maintenance.
How Does Healix 360 Facilitate Personalized Wound Care and Referrals?
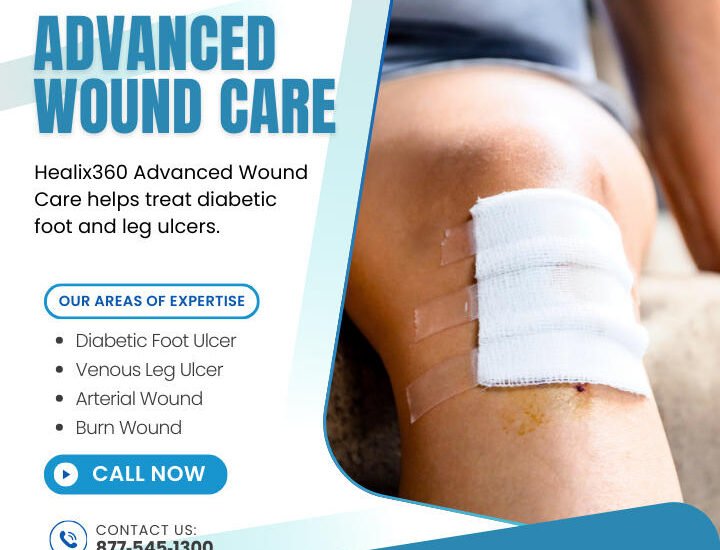
Healix 360 specializes in providing personalized wound care solutions tailored to individual patient needs. With a focus on advanced wound dressing selection and healing solutions, Healix 360 offers both in-clinic and private residence care. Their team of board-certified specialists works closely with patients to develop customized treatment plans for chronic wounds, diabetic ulcers, and pressure injuries. This patient-centered approach ensures that each individual receives the most effective care possible.
What Educational Materials and Tools Are Available for Optimal Dressing Choice?
Healix 360 provides a range of educational materials and tools designed to assist patients and providers in making informed decisions about wound dressing selection. These resources include informative articles, instructional videos, and access to specialists who can offer guidance on the best dressing options for specific wound types. By leveraging these tools, patients can enhance their understanding of wound care and improve their healing outcomes.
For patients requiring specialized attention in a comfortable setting, private residence care offers a tailored approach to wound management.
To learn more about specific conditions and treatment options, visit our conditions page.